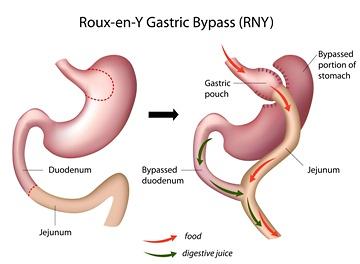
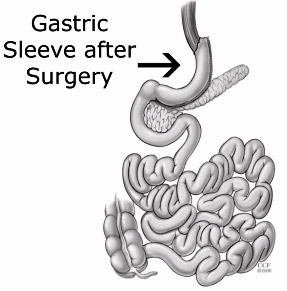
Introduction
During the last decades, obesity has become a major health care concern. Moreover, obesity is related to different comorbidities as coronary heart disease, hypertension, insulin resistance, type 2 diabetes, hyperlipidemia, obstructive sleep apnea, muscular and joint pain, degenerative osteoarthritis, and depression. These comorbidities not only lead to a reduction in life expectancy, but also in quality of life. The accumulating evidence identifying obesity-related mortality and comorbidities is an important factor that has led to increased numbers of patients seeking treatment through bariatric surgery. Many different approaches (diets, exercise, and pharmacologic treatments) have been proposed to treat patients with morbid obesity but with a high failure rate, only bariatric surgery showed excellent short- and long-term results. Bariatric surgery produces body weight loss ranging from 50% to 75% of excess body weight, and these results are constant during a long-term follow-up period. Although behavioral and pharmacologic treatments of obesity can result in short-term body weight loss of approximately 5% to 10% body weight (with some of the most successful studies reporting body weight loss as great as 18.8% at 12 months), they have not been able to produce more than a modest body weight loss for most patients. Nor have these treatments demonstrated long-term success. In addition, weight loss is maintained longer after bariatric surgery than after nonsurgical treatment of obesity. Laparoscopic Roux-en-Y gastric bypass (LRYGB) is currently considered the gold standard for morbid obesity; it is a restrictive and malabsorptive irreversible procedure, first reported by Wittgrove and Clark in 1994. It is a technically demanding procedure with a long learning curve and a considerable morbidity and mortality rate.Observational retrospective study from a prospective database of patients undergoing LRYGB and LSG between 2004 and 2011, where 249 patients (mean age 44.7 years) were included. Patients were followed at 1, 3, 6, 12, and 18 months, and annually thereafter. Short- and mid-term weight loss, comorbidity improvement or resolution, postoperative complications, re-interventions, and mortality were evaluated. Patients were evaluated and followed pre- and perioperatively by a multidisciplinary team (surgeons, endocrinologist, psychologist, psychiatrist, dietitians, and anesthesiologist).
Discussion
In this study, both LSG and LRYGB were safe and effective bariatric procedures resulting in significant weight loss and favorable effects on comorbidities. LSG is technically less complex that that with the LRYGB, which is reflected by a lower operative time (153 min LRYGB vs. 93 min LSG, p< 0.001) and shorter length of stay (4 vs. 3 days in LRYGB and LSG, respectively; p>0.001).
With respect to %EWL, a %EWL over 65 % with both techniques 4 years after surgery can be obtained, without significant differences between LRYGB and LSG. Results available in the literature showed a wide range of %EWL from 33 to 83%. In our study, more than 80 % of patients were followed for at least 4 years.
When patients with more than 50 % of %EWL were analyzed, there were no differences between LRYGB and LSG at 1 year (95.4 vs. 90.8 %) and 4 years (90.4 vs. 80 %). Some factors have been proposed to have influence in the %EWL in LSG. Bougie sizes ranging from 32 to 60 F have been studied, but not direct correlation with %EWL has been demonstrated. The distance from the pylorus to the beginning of the gastric transection and the complete resection of the fundus responsible for the ghrelin secretion have been also proposed as factors influencing the results. However, there was no broad agreement on these technical aspects. In our study, the same maneuvers were used in all patients: a 36-F bougie, 5 cm from the pylorus to the initiation of gastric transection, and the complete resection of the fundus. We take especially care in the dissection of the left crus, the identification of the fat pad and the dissection of the posterior attachments from the stomach to the pancreas to facilitate the complete resection of the fundus and avoid any remnant that may cause failure as has been suggested by several authors. Perhaps this combination may account for the excellent results obtained with LSG.
Although most of the data available suggest that morbidity related to LSG is lower than in LRYGB, results show a disparity. Our results confirm that morbidity is significantly lower in patients undergoing LSG, although these figures are related to a higher number of minor complications (20 vs. 3.5 %) but not to the incidence of major complications (5.9 vs. 4.4 %). Six gastric leaks were observed in the whole series (3 [2.2 %] in the LRYGB group and 3 [2.9 %] in the LSG).
All leaks in the LRYGB were treated by conservative measures (endoscopic or medical) whereas two in the LSG needed surgery. As expected, morbidity prolonged hospital stay in our study, but had no influence in the mortality rate.
Nine patients required re-intervention [6 (4.4 %) of the LRYGB group and three (3.5 %) of the LSG group]. Hemorrhage was the cause of 50 % of the revisions in our series, mostly due to port-site bleeding. Since 2008, our policy is to systematically close all 10-mm port-sites and in the last 161 cases we have not needed any further re operation for this reason. Also, we recently started using stapler reinforcement with buttress material. There was no mortality directly related to the surgical procedure and the readmission rate was lower than in other studies with no differences between LRYGB and LSG. As with others, we showed an improvement of comorbidities that may become higher than 95 % in diabetes mellitus or obstructive sleep apnea. There are few data in the literature comparing results between LRYGB and LSG, but the present data confirm similar improvement rate with both surgical techniques. Regarding the metabolic profiles, the impact of LRYGB is well-known but few data are available with LSG. A previous report of our group demonstrates that LRYGB and LSG markedly improved glucose homeostasis. LSG decreased fasting and postprandial ghrelin levels, whereas GLP-1 and PYY levels increased similarly after both procedures. Reduced ghrelin levels after LSG could be responsible of the weight-reducing effect LSG. Moreover, we also demonstrated that bariatric surgery reduces 50 % the estimated cardiovascular risk at 1 year after surgery and that LSG is equally effective as LRYGB except for cholesterol metabolism.
Conclusion
One hundred thirty-five LRYGB and 114 LSG were included. Significant statistical differences between LRYGB and LSG were found in operative time (153 vs. 93 min. p< 0.001), minor postoperative complications (21.5 % vs. 4.4 %, p00.005), blood transfusions (8.8 % vs. 1.7 %, p= 0.015), and length of hospital stay (4 vs. 3 days, p<0.001). There were no differences regarding major complications and re-interventions. There was no surgery-related mortality. The percentage of excess weight loss up to 4 years was similar in both groups (66±13.7 vs. 65±14.9 %). Both techniques showed similar results in comorbidities improvement or resolution at 1 year.
In conclusion, both LRYGB and LSG are safe procedures that provide excellent results in weight control and resolution of comorbidities in patients with morbid obesity. On the whole, many doctors today recommend gastric sleeve as a faster, less expensive, and more effective weight loss procedure with lower complication rates, and so do we.
References
1. P. Vidal, J.M. Ramón, A. Goday, et al., “Laparoscopic Gastric Bypass versus Laparoscopic Sleeve Gastrectomy as a Definitive Surgical Procedure for Morbid Obesity. Mid-Term Results”, OBES SURG (2013), 23:292–299.
2. F. Abbatini, M. Rizzello, G. Casella, et al., “Long-term effects of laparoscopic sleeve gastrectomy, gastric bypass, and adjustable gastric banding on type 2 diabetes”, Surg Endosc (2010), 24:1005–1010.
3. C. Arthur, et al., “The Comparative Effectiveness of Sleeve Gastrectomy, Gastric Bypass, and Adjustable Gastric Banding Procedures for the Treatment of Morbid Obesity”, Annals of Surgery (2013), 257(5): 791–797.