Comparison between Gastric Bypass and Gastric Banding Bariatric Surgeries
2 Oct, 2013Robotic Sleeve Gastrectomy versus Laparoscopic Sleeve Gastrectomy: a Comparative Study with 200 Patients
3 May, 2014Transanal Endoscopic Microsurgery (TEM)
Rectum surgery methods
There are two categories of surgeries available for Rectum disorders including Radical (open or major) and local surgeries. The former group, by making major incisions, opens up the area of the surgery and provide a wide view and space for the surgeon to perform the operation, but the rate of after-surgery complications as well as dysfunction of the involved organs is high in these surgeries. Therefore, for benign rectal disorders invention of less invasive local techniques has been considered. Of these local surgery techniques conventional transanal endoscopy and the novel method of transanal endoscopic microsurgery could be named.
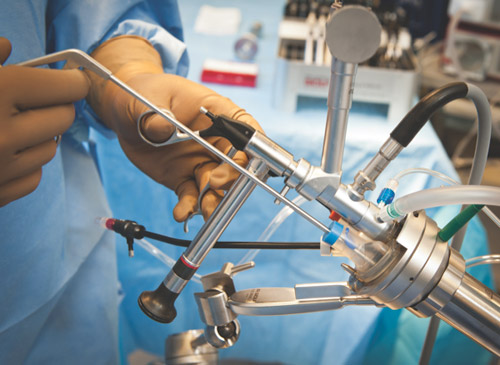
Transanal Endoscopic Microsurgery (TEM)
Transanal endoscopic microsurgery (TEM) came into practice in Germany, in the early 1980s. Its initial indication was to remove large rectal polyps beyond the reach of standard transanal excision. TEM is a technique for the performance of local excision, by the way of a binocular, magnified operating system. This equipment involves an operating proctoscope, insufflation, and magnified stereoscopic vision. In fact, the three-dimensional amplification, magnified stereoscopic view and lighting within the rectal lumen, allow excellent vision of the operative field, enabling the surgeon to perform an extremely precise excision of rectal lesions, including a full-thickness excision. It has evolved into a valuable, state-of-the-art technology equaling any other technique in terms of reliably positive patient outcome. Its application has expanded beyond the excision of colonoscopically unresectable polyps to the removal of select, early rectal cancers, independent of prior adjuvant chemoradiation therapy. TEM has been found useful in the treatment of a broad variety of disease processes, both benign and malignant. Though many indications have been described, including excision of carcinoids or even retrorectal tumors, the most common use of TEM remains the resection of colonoscopically unresectable rectal adenomas and carefully selected rectal cancers. It should be stressed that even though TEM extends the reach of conventional transanal resections, it should not lead to any deviation from the established stringent indications for resection, especially in regard to rectal cancer.
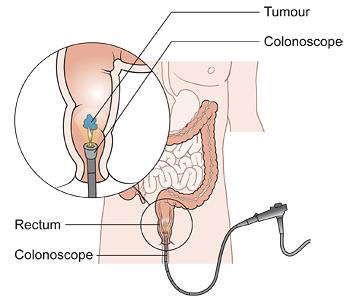
Surgical technique
Preceding the procedure, bowel cleansing and prophylactic antibiosis have to be performed. In the actual procedure, two different operation techniques can be employed. Mucosectomy involves removing the mucosa, including the polyp from the inner circular layer of the muscularis; it represents a suitable technique for sessile adenomas located in the intraperitoneal portion of the rectum. Full-thickness excision requires removal of all layers of the rectal wall, in the plane located just slightly superficial of the perirectal fatty tissue. This excision is performed for the majority of malignant lesions. In cases of malignancy, it is imperative that the procedure includes not only a full-thickness excision but also a 1 cm safety margin of normal mucosa surrounding the lesion.
Current indications and results
Results from various experiences are evaluated in the following chapter
TEM for benign lesions
Benign rectal tumors that are not suitable for snare diathermy excision are often amenable to removal via the transanal route, employing anal retractors and Parks’s method. However, this method is limited to the lower third of the rectum. In addition, it may be difficult to visualize the margins of flat adenomas. Conventional management of higher rectallesions usually involves transabdominal procedures, posterior trans-sacral, orsphincter-splitting approaches. However, these are major surgical procedures with associated complications and may be unsuitable and unnecessary if the purpose of the intervention is to resect benign lesions or low risk carcinomas. With the development of TEM by G. Buess, it is now possible to carry out formal transanal resection by means of a rectoscope, which affords excellent access and vision in the entire rectum. Some surgeons recommend a full-thickness resection, to ensure an appropriate margin of safety. In addition, it is claimed that this standard procedure is technically easier to perform than mucosectomy and that it decreases the risk of missing a small rectal cancer which may be located within the villous adenoma. Such ‘intraephitelial neoplasia ⁄dysplasia’ or ‘early invasion’ has been reported in up to 31% of cases. Although it is often difficult to ascertain the precise techniques (full-thickness or submucosal) used, the rates of complete excision at the time of operation and the exact follow up, large published series report a rate of recurrences in up to 27.3% after transanal excision of rectal adenomas. In contrast the results reported using TEM show a recurrence rate between 3 and 7% with the 5.6% for the adenoma cases of a series published in 2004, being well in accordance with previous studies. The overall morbidity rate for conventional transanal surgery in reported series varies from 0 to 14.5%, compared with 6% reported in the largest series of a total of 318 adenomas treated by Mentges. These results are in accordance with others TEM series reporting morbidity of up to 4.5% in more than seven hundred patients. It is of interest that postoperative bleeding is unusual with TEM, whereas it accounts for over half of the complications reported in other series. Peritoneal entry, on the other hand, as assessed intra-operatively in 8 patient of an experience (two of them with postoperative pneumoperitoneum), can be a significant source of morbidity with TEM. Presumably the excellent vision afforded by TEM allows more precise haemostasis, whereas the ability to excise high rectal lesions increases the likelihood of peritoneal entry, especially when the tumour is anterior, and thus more likely to be above the peritoneal reflection. Perforations could be recognized and managed by immediate endorectal suture. The results of a study, after initial 100 cases with TEM, indicate that this technique is reproducible with suitable surgical training. Interestingly all three protective ileostomies in that series occurred within the first 20 cases indicating a learning curve, despite the fact that all surgeons received a special TEM training. Regarding the effect of a prolonged anal dilatation with the 40 mm diameter TEM operative rectoscope, manometric studies indicate a decrease in anal sphincter tone ranging from 25% to 37% of pre-operative sphincter pressure, with recovery to clinical continence within 6–16 weeks. One study observed postoperative transitory grade II incontinence in 65 of the 100 patients, with full recovery in 98%of the cases after 12 weeks. There is also evidence indicating a significantly increased risk of diminishing the anal resting pressure by procedures lasting more than two hours. Others found 21% disturbances of rectoanal coordination and rectal perception, depending on the extent and type of resection of the tumor. However, when making continence judgement, it would be necessary to consider the risk of incontinence by using the Parks retractor in conventional surgery, or after a low restorative rectal excision, if those were to be the alternative procedures. In conclusion, TEM as a minimally invasive technique might be expected not only to benefit a small, specific population of patients in terms of morbidity but also to improve results in terms of completeness of excision and recurrence rates when compared to conventional transanal resection.
TEM for early rectal cancer
The standard treatment for early rectal cancer has been major surgery by anterior or abdominoperineal resection. After the introduction of total mesorectal excision, results regarding recurrence and survival rates have improved dramatically. However, mortality, morbidity, and functional disturbances after major surgery are considerable. Perioperative mortality rates are usually 2 to 3 percent and overall morbidity 20 to 30 percent. Furthermore, anorectal, bladder, and sexual function may be compromised. Given these side effects, there has been an increasing interest in the locoregional treatment of early rectal cancer. Nowadays local excision for selected rectal neoplasms is an accepted treatment worldwide. Compared to the gold standard of radical surgery, local procedures of strictly selected early rectal cancers should lead to identical oncological results and even better outcomes regarding morbidity, mortality, and quality of life. Regardless of this trend, conventional transanal excision of rectal cancer has recently come under close scrutiny because of relatively high rates of local recurrence. In fact, scepticism has been expressed that such treatment may not be in the patient’s best interest. Despite all these concerns transanal endoscopic microsurgery has become the current standard procedure for the treatment of large rectal adenomas and early low risk carcinomas with curative intent, mostly in Europe. As already assessed and in contrast to conventional transanal excisions using anal retractors, TEM offers an exceptionally good overview of the whole rectal cavity, allowing the precise removal of lesions not only in the lower and middle rectum but also in the upper region or even the retrorectal space, and obviates the need for major surgery. Despite the limitations and the lack of power of clinical studies to detect differences in outcome such as survival and complication rates, TEM does appear to result in less local recurrence than other usual methods of local excision. Furthermore, after local excision of early rectal cancer by TEM, recurrence and survival rates are comparable to those seen after major surgery, and complication rates and functional results are even superior when put into contrast with those seen after major surgery. Since the introduction of TEM a majority of patients with adenomas and T1 low-risk rectal cancer have been treated with local excision by this technique. In 2009 we ran a single center report to evaluate the safety and oncological outcomes of TEM excision compared to radical surgery (RS) in the treatment of T1 low-risk rectal cancer. We found no statistical differences between RS and TEM in terms of local recurrence and disease free survival rates. Today, various surgical techniques are still under discussion for the treatment of early rectal carcinomas. The historical gold standard procedures, such as anterior and abdominoperineal resection, show excellent results regarding local recurrence and survival rates, but are dearly paid for by a high incidence of complications and impaired quality of life (anorectal, sexual, and urinary dysfunction). Additionally, some of the patients require temporary diverting enterostomies. On the other hand, there are conventional, sphincterpreserving techniques, such as conventional transanal resection with Park’s retractor, which are associated with an almost unacceptably high local recurrence rate of up to 29%. The primary factor limiting the effectiveness of local treatment for early rectal cancer is lymph node invasion. Depths of invasion into the rectal wall, grade or degree of differentiation, vascular, lymphatic and neural invasion are independent predictors of the risk of nodal metastasis. Since initial studies by Morson and Hermanek large series of resected rectal cancers have shown that well-differentiated tumors confined to the submucosa (T1) without vascular, lymphatic or neural invasion carry a 4% risk of nodal metastasis. Although the reported rate of recurrence for early rectal cancers (pT1) resected by TEM is between 4- and 14%, follow-up and differentiation between low- and high-risk features are variable among series reported. In fact, the only published prospective study comparing TEM with radical resection for T1 low risk rectal cancer showed no statistical difference between local excision and radical resection regarding local recurrence and metastasis rate. These results are in accordance with astudy that assessed two recurrences in the TEM group compared to none in the RS group. Local control is therefore undoubtedly better assessed after RS, but on the other hand it is interesting to underline that there was no statistically significant difference in overall survival and disease-free survival depending on the operation performed. In an outstanding systematic review published recently, both comparative and case-series studies were examined to assess evidence related to the safety and efficacy of TEM compared with radical resections and conventional local excisions. Despite limited evidence the authors pointed out the unequivocal tendency of TEM to achieve better results in well-selected cases than conventional local excision, without being less effective than radical resection. The question arising is, whether TEM represents the only adequate alternative to radical resection for early rectal cancer. The reason for the superiority of TEM over other transanal conventional techniques is the use of an optical system with 3D-view, 6-fold magnification, and human eye resolution; the creation of a stable pneumorectum, and specially designed instruments that allow full thickness excision under excellent view conditions not only in the lower but also in the middle and upper parts of the rectum. Furthermore, full-thickness excision allows proper histological examination. Recently we showed the ability and advantages of this technique to approach tumors located in the retrorectal space. The advantage of TEM has already been observed in the lower rate of recurrences for adenoma excision (up to 7%) when compared to recurrence rate after transanal conventional excision (up to 27.3%). Even for adenomas, completeness of excision is an important predictor for early recurrence. Furthermore, the literature reported a lower morbidity rate when using TEM for adenoma excision (7% complication rate compared to 14.5% for conventional transanal surgery). Surprisingly many publications still advocate for caution in the local excision of rectal cancer. However, these studies are questionable regarding selection criteria, use of endorectal ultrasounds preoperatively, proper “in toto” excision, and histological examination (R-Status, differentiation, and lymphovascular invasion). In addition, some data is compromised by mainly retrospective analyses over extended time periods, and by a lack of standardized pathology reports. The main argument explaining the high rate of local recurrences after conventional local excision could be a technically inadequate operation in which margins are insufficient, inadequate depth of resection, or shedding and implantation of tumor cells into the surgical field. Moore compared 82 patients after TEM with another 89 after conventional transanal excision for rectal neoplasms. He found clear margins in 71 percent of specimens in the conventional group compared with 90% in the TEM group. Furthermore, non-fragmented specimens were more likely to be found after TEM than after conventional surgery (94 vs. 65 percent). In another study the rate of Rx and R1 after local excision was 5.88 and 2.94%, respectively. We believe that strict patient selection criteria, together with full-thickness and margin-free excision is crucial for patient outcome. The strong correlation between incomplete tumor resection and poor outcome is widely accepted. In another experience, positive excision margins should not be regarded as a risk factor for recurrence but should be viewed as insufficient therapy requiring further treatment.
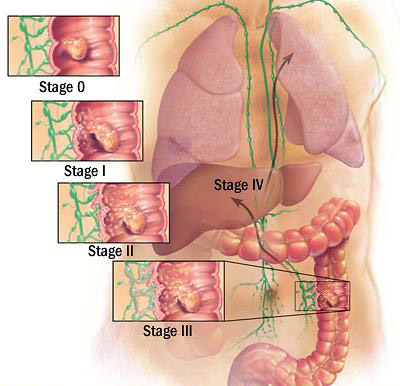
TEM in rectal cancer after chemoradiation
Although adjuvant or neoadjuvant chemoradiotherapy seems to improve the prognosis after local excision, the indications for any kind of therapy following local resection of rectal cancer by TEM remain controversial. In fact, local treatment of rectal cancer is limited by the impossibility of removing the potentially positive lymph nodes, supporting the concept of adjuvant radiotherapy, chemotherapy, or both to achieve local control of the lymph nodes. Borschitz published a review of the findings of neoadjuvant chemoradiation (nCRT) and local excision (LE) for T2–3 rectal carcinoma. He found a total of 237 patients in seven different studies available for analysis, which did in fact permit an assessment of the recurrence rates in relation to histopathological tumor response. Patients with systemic metastases were excluded, and lymph node status was provided by only a few authors. In most studies analysed, clinical staging before nCRT identified a T2/3 rectal carcinoma (T1 2%; T1–2 14%; T2 34%; T3 50%). The studies reported different therapeutic concepts, tumor locations, and intervals from completion of nCRT to surgery. Nevertheless, the analysis by Borschitz identified a number of similarities among them. These were predominance of cT2–3 carcinomas and the occurrences of local recurrence (LR). Patients with response at the submucosa level (ypT1) consistently showed low LR rates of 2% (0%–6%). Less clearly defined were the results of ypT2 findings, which ranged from 6% to 20% LR rates. Clearly unfavorable were the findings in patients, whose disease did not respond to therapy (ypT3), for whom a mean LR rate of 21% was calculated. The widely divergent LR rates of ypT2 findings may be increased as a result of to nonuniform time intervals from nCRT to surgery. The study by Borschitz confirms prior findings observed after nCRT and conventional resection. Almost no LR were reported for CR after nCRT of advanced (T3/4) tumors. Critical prognostic parameters are tumor response and tumor- free lymph nodes. LR and systemic recurrence rates ranging 0% to 23% and 8% to 22% were determined for this constellation. For lesions that did not respond to therapy and for persistent nodal disease, far higher LR rates ranging from 16% to 58%, and metastases ranging from 35% to 58% were reported. Neoadjuvant CRT followed by LE may represent a viable alternative to rectum extirpation in patients with low T2–3 rectal carcinoma. Despite an optimized surgical technique made available by total mesorectal excision, less favorable results were reported for tumors in the lower rectum. The distal mesorectum, described by Morson as a ‘‘bare area,’’ attenuates distally and is characterized by a circumferential decrease in healthy tissue surrounding the tumor, leading to a loss of tissue layers and a restricted field of view. For this region, incomplete mesorectal excision has been suggested as the cause of higher LR rates. Local full-thickness excision may be performed as an adequate therapeutic measure for complete response (CR) after nCRT. The described concept has been taken one stepfurther by Habr-Gama who did not find a need for subsequent surgery in patients with clinically complete responses. In her retrospective, long-term, follow-up study which so far has remained unique, she reports a LR rate of only 3% in 100 patients. The question whether radical surgery, LE, or close-meshed follow-up alone may be appropriate in these patients, still remains largely unanswered. Furtherly, it needs to be clarified, whether after nCRT with clinical confirmation of complete response, possibly remaining but vital tumor cells require surgical removal. These cells may have been damaged by irradiation and thus rendered unable to proliferate. Alternatively, some tumor cells surviving nCRT may represent resistant hypoxic clones that build the basis for development of recurrence later on. In summary, the findings of the revision made by Borschitz support the proposition that the indication for LE after nCRT may be extended to distal cT2–3 rectal carcinoma. The strongest prognostic parameter for favorable oncological outcomes is an effective tumor response without residual tumor (ypT0) or with response to at least the submucosa level (ypT1) in the excised specimen. For ypT2 tumors, the interpretation of the heterogeneous results should be performed with caution. But an extrapolation may be possible from LE alone, without nCRT. LE is not adequate in patients whose tumors exhibit no response or weak response to nCRT. These patients should be treated conventionally, that is, using radical surgery.
Conclusion
Transanal Endoscopic Microsurgery is a fairly new variant of transanally performed surgery of the rectal cavity, developed in Germany during the 1980’s. In comparison to preceding techniques, it has largely expanded the spatial range and resolution of transanal procedures by employing state-of-the-art optics and endoscopic instruments, enabling the surgeon to reach parts of the rectum that were previously inaccessible by transanal approach. Repassing the findings throughout the manuscript, it is evidence based to conclude that TEM currently is and prospectively will be playing an important role in the management of lower rectal neoformations. When used in select cases of adenoma or low-grade adenocarcinoma and in accordance with the stringent indications governing more radical interventions, already in-place, patients are due to benefit from less morbidity and mortality, including shorter recovery times. Within its constraints, TEM has also shown a more favorable incidence of local recurrences compared to standard transanal surgery, while being able to parallel local recurrence rates of more extended invasive interventions, like anterior resection and abdominoperineal approaches, outlining its qualities in curative treatment of rectal cancer. It has to be stressed, that the suitability of TEM must be determined in a meticulous preoperative staging and grading process, including MRI imaging and endorectal ultrasound, to tackle the thin red line separating available approaches case by case. Apart from that, TEM may also serve as a last line measure for patients unfit or unwilling to undergo laparotomy, adding to its value in managing palliative instances. Additionally, in multimodal therapy schemes, including neoadjuvant chemoradiotherapy, the indication of TEM could expand, in the near future, to those patients showing a complete response.
Reference
P. Palma, K. Horisberger, Transanal Endoscopic Microsurgery- State of the Art, Therapeutic Gastrointestinal Endoscopy, Prof. Oliviu Pascu (Ed.), ISBN: 978-953-307-743-7, InTech, 2011.
