Klatskin tumor
13 Jan, 2016MMESA Spring Meeting 2016
26 May, 2016The History of Sleeve Gastrectomy
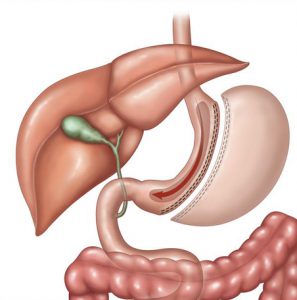
The sleeve gastrectomy is rapidly emerging as a reasonable alternative to adjustable gastric banding and other stapling procedures. Its earliest development was in anti-reflux surgery, and it was originally the restrictive component of the duodenal switch. The laparoscopic approach and the evolution of a reduced pouch volume have demonstrated results comparable to other stapling procedures both with weight loss and safety.
The sleeve gastrectomy (Figure 1) is a purely restrictive procedure, meaning there is no intestinal bypass. It may also have a “resective” or “reductive” quality in that a large portion of the stomach is removed, which may facilitate gastric emptying and favorably alter duodenal and ileal gut hormones. The gastric reduction may also reduce the amount of ghrelin and related hormones that are released, which may also provide a hormonal advantage to help reduce caloric intake.
The history of the sleeve gastrectomy is more an evolution of prior procedures than a discrete timeline of development of a single procedure. The procedure has its roots in the earliest gastroplasty procedures and as an observation from prior anti-reflux procedures. It was Doug Hess, in Bowling Green, Ohio, who performed the first open sleeve gastrectomy in March of 1988 as part of what is now known as the duodenal switch procedure (Figure 2).[1,2] Lawrence L. Tretbar described weight loss associated with a fundoplication for reflux surgery. He described an extension of the fundoplication that created a tubular structure that achieves weight loss (Figure 3).
In a series of 20 patients with 1- to 16-month follow up, weight loss ranged from 15 pounds at one month up to 55 pounds at 16 months.[3]
Dr. Hess used this concept of a tubular stomach and modified from an extended plication to an actual longitudinal or vertical gastrectomy. (Figure 2). This type of gastrectomy that also left in place the first portion of the duodenum helped solve the problem of dumping symptoms and marginal ulcers seen with the Scopinaro bilopancreatic diversion. This was because an intact pylorus was left and a duodenal enteric anastomosis was performed instead of a gastro-enteric anastomosis.
In 1997, the author of this article (GA) was performing an open duodenal switch on a 13-year-old girl with a history of common bile duct stones.[4] Intraoperatively, the common bile duct stones could not be completely cleared. Therefore, he elected to limit the procedure to just an open sleeve gastrectomy in order to leave access for a postoperative endoscopic retrograde cholangiopancreatography (ERCP). From 1997 to 2001, he performed 21 open sleeve gastrectomies in high-risk patients with super-morbid obesity. The pouch was approximately 100mL in volume (currently pouch volume is approximately 50cc or less) and the patients achieved 40- to 50-percent excess weight loss (EWL). By October 2005, he had reported on 118 open sleeve gastrectomies with similar results.[5]
In 1999, the first laparoscopic approach to the duodenal switch was developed on a porcine model by deCsepel, Jossart, and Gagner.[6] The sleeve gastrectomy portion of the procedure was found to be feasible. Gagner proceeded with the laparoscopic duodenal switch on humans but noted a high complication rate in the higher body mass index (BMI) group.[7] He subsequently developed the technique of staging the intestinal bypass procedure by performing the laparoscopic sleeve gastrectomy first as an initial stage.8 From 2001 to 2003, seven patients with a BMI of 58 to 71kg/m[2] underwent a first stage sleeve gastrectomy with a subsequent Roux-en-Y gastric bypass. The average EWL was 37kg (33%EWL) and this allowed for a safer second stage. These preliminary results quickly popularized the procedure as a safer laparoscopic option for the higher BMI group.
In San Francisco, our group had noted the good results from the Magenstrasse and Mill procedure (Figure 4) published by Johnston et al.[9] There were 100 patients with a five-year follow up and 60-percent EWL. This group tended to have a BMI between 35 and 50 and the best pouch volume was 32 French in caliber. We recognized that our duodenal switch patients with larger pouches did not have optimal weight loss due to inadequate restriction, so we started to offer the sleeve gastrectomy with a 32 French caliber pouch (30-60cc) to lower BMI patients.[10] The results in our first 216 patients compared favorably to the other stapling procedures and adjustable gastric banding with 75- to 85-percent EWL at two years of follow up. Currently, our series has more than 1,300 patients, and we now have limited data at four years. The four-year percent EWL is 68 percent for the BMI group less than 55 kg/m[2] (n=23) and 59 perent for the BMI group greater than 55 kg/m[2] (n=16). The limited number of patients at four-year follow up is due to our reluctance to widely recommend this procedure during our early experience. In 2010, we have more than 200 patients achieving the five-year mark and, to date, these results appear stable. Results presented at the 2nd International Consensus Conference in Miami in March 2009 revealed five-year weight loss results in a limited number of patients ranging from 42 to 80 percent EWL.[11]
In summary, the sleeve gastrectomy has evolved from an open duodenal switch procedure to an open sleeve gastrectomy to a laparoscopic sleeve gastrectomy. The earliest experience was in higher risk patients with super-morbid obesity as a safer staged procedure but this quickly developed into a single-stage option for lower BMI patients. The reason this procedure is safer in higher BMI patients is because the lack of an intestinal bypass eliminates the issue of anastamotic tension and dehiscence; the procedure can be done faster; and the procedure is more likely to be completed laparoscopically. The intraoperative and early postoperative safety in the lower BMI group may not be superior to a RYGB because reported leak rates are typically between 1 and 3 percent. However, the long-term safety of this procedure is definite as there is essentially no risk of marginal ulcer or small intestinal obstruction, which does occur with the gastric bypass.
There are at least two main issues that will hopefully be resolved over the next few years. The first is a standardized pouch volume. Most surgeons are migrating toward a smaller pouch volume (30–40cc) and leaving less antrum to allow for a more durable weight loss as it is believed the smaller diameter pouch is less likely to dilate over time. Unfortunately, this smaller volume increases the chance of staple line bleeding and dehiscence, especially near the gastroesophageal junction. Proper management of the staple line with buttress materials, suture inversion, and fibrin sealants will ultimately optimize the safety of this procedure.
References:
2. DeMeester TR, Fuchs KH, Ball CS, et al. Experimental and clinical results with proximal end-to-end duodeno-jejunostomy for pathologic duodenogastric reflux. Ann Surg. 1987;206:414–424.
3. Tretbar LL, Taylor TL, Sifer EC. Weight reduction. Gastric placation for morbid obesity. J Kans Med Soc. 1976;77(11):488–490.
4. Almogy G, Crookes PF, Anthone GJ. Longitudinal gastrectomy as a treatment for the high-risk super-obese patient. Obes Surg. 2004;14:492–497.
5. Hamoui H, Anthone GJ, Kaufman HS, Crookes PF. Sleeve gastrectomy in the high-risk patient. Obes Surg. 2006;16:1445–1449.
6. DeCsepel J, Burpee S, Jossart GJ, et al. Laparoscopic biliopancreatic diversion with a duodenal switch for morbid obesity: a feasibility study in pigs. J Laparoendosc Adv Surg Tech A. 2001;11(2):79–83.
7. Kim WW, Gagner M, Kini S, et al. Laparoscopic vs. open biliopancreatic diversion with a duodenal switch: a comparative study. J Gastrointest Surg. 2003;7(4):552–557.
8. Regan JP, Inabnet WB, Gagner M. Early experience with two-stage laparoscopic roux-en-Y gastric bypass as an alternative in the super-super obese patient. Obes Surg. 2003;13:861–864.
9. Johnston D, Dachtler J, Sue-Ling HM, et al. The Magenstrasse and Mill operation for morbid obesity. Obes Surg. 2003;13(2):318.
10. Lee CM, Cirangle PT, Jossart GH. Vertical gastrectomy for morbid obesity in 216 patients: report of two-year results. Surg Endosc. 2007; 21(10):1810–1816.
11. Weiner, Himpens, Schauer, McMahon. Discussion. The Second International Consensus Summit for Sleeve Gastrectomy, March 19–21, 2009..
