Learning course and Animal Lab on TachoSil
2 Mar, 2013Transanal Endoscopic Microsurgery (TEM)
23 Oct, 2013Bariatric Surgeries
Obesity type 3, defined as a body mass index (BMI) of greater than 40 kg/m2 is increasing worldwide. This disease is associated with premature death and an increased risk for diabetes, hypertension, hypercholesterolemia, heart disease, osteoarthritis, sleep apnea and gallbladder disease. Previous research has shown that weight loss improves both social functioning and quality of life. Carefully controlled studies have demonstrated between 25% and 60% reductions in all-cause, cardiovascular and cancer mortality associated with significant weight loss. Due to the fact that primary solutions like low calorie diets, exercise and medications usually are not very effective for high degrees of overweight (the permanent weight loss they yield is 4 to 7kg), the rate of bariatric surgeries is increasing such that it has been 10-folded in the recent 2 decades. The surgeries are usually more effective and their results last longer. National and international Health institutes usually suggest these surgeries for people with BMI>35 or 40 kg/m2.
The two most commonly used bariatric surgeries are Gastric Bypass Roux-en-Y and Gastric Banding which are to be compared in this article.
Description
Gastric Banding
It is a restrictive procedure during which an inflatable band is placed around the upper part of the stomach. This creates a smaller stomach pouch, which restricts the amount of food that can be consumed at one time and increases the time it takes for the stomach to empty. As a result, a patient achieves sustained weight loss by limiting food intake, reducing appetite, and slowing digestion. Hereinafter this surgery is called banding, for short.
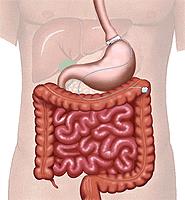
Gastric ByPass
It is a combination procedure that uses both restrictive and malabsorptive elements. First the stomach is stapled to make a smaller pouch. Then most of the stomach and part of the intestines are bypassed by attaching (usually stapling) a part of the intestine to the small stomach pouch. As a result, a patient cannot eat as much and absorbs fewer nutrients and calories. Hereinafter this surgery is called bypass, for short.
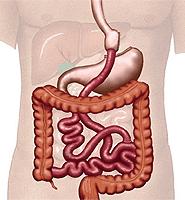
What do statistics and research studies say?
It has been observed that during the first year after surgery, the weight loss caused by Bypass is 25% higher than banding. While some surgeons have reported that in five years the results of the two methods is comparable (55% over-weight loss for banding compared to 59% for bypass), others have reported a significant long-term differences as well. In addition, it can be inferred from most studies that the effect of surgery on the resolution of comorbidities is 25% higher in bypass; which means that from every 4 people who undergo bypass instead of banding, one person would relieve from the comorbidities (i.e. heart disease, diabetics, etc.). There are also some researches that consider the two methods comparable in this regard as well. Besides, long-term complications like need for reoperations are less in bypass (14% to 17%).
On the other hand, banding surgery procedure is less complicated and minimally invasive. The duration of surgery is 68 minutes, hospital times about 2 days and complete recovery time is about a week less in banding. Also the evidences indicate that short-time complications as well as mortality rate is less in banding surgery (0.06% to 0.17% mortality rate), although mortality rate is small for both procedures. General complications aroused by surgeries are comparable in two procedures. Overall it has been shown that short-term effects of banding surgery is 1.1% to 6.3% less in banding.
Patient Satisfaction
Only 1 comparative study reported data on patient satisfaction. Approximately 80% of the patients in bypass group reported being very satisfied with the procedure and no patients in this group were unsatisfied or regretted having had the procedure. In contrast, only 46% of the patients who underwent banding surgery reported high satisfaction while 19% of them were totally unsatisfied or even regretting.
High quality studies
One of the most comprehensive and accurate studies focused on comparison of the two procedures published in 2006 investigated 181 patients matched for age, sex, BMI and surgery date. The over-weight loss ate the first year was 76% for bypass compared to 48% for banding and the results persisted for 3 years. It also was seen that in 78% of people who also suffered from diabetes the comorbidity was cured. This was while the rate was 50% for banding. The need for reoperations was 19% for bypass versus 24% for banding. No deaths were reported in this study.
A new comprehensive study published in 2012 reported that follow-up was 92.3% at the end of the study period (6 years postoperatively). Early morbidity was higher after bypass than after banding (17.2% vs 5.4%), but major morbidity was similar. Weight loss was quicker, maximal weight loss was greater, and weight loss remained significantly better after bypass until the sixth postoperative year. At 6 years, there were more failures (BMI>35 or reversal of the procedure/conversion) after banding (48.3% vs 12.3%). There were more long-term complications (41.6% vs 19%) and more reoperations (26.7% vs 12.7%) after banding. Comorbidities improved more after bypass.
General comparison
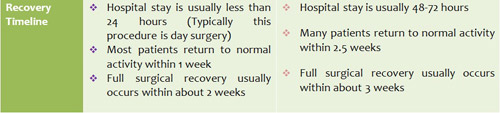
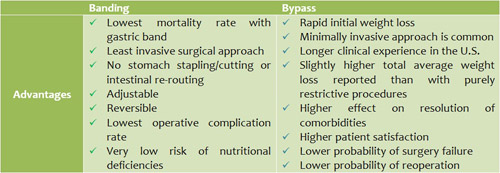
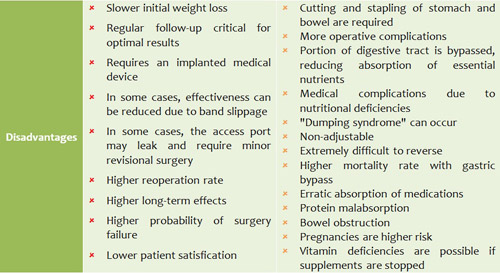
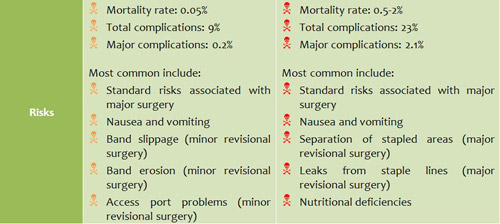

Discussion and Summary
The studies up to now clearly indicates that during the first year after surgery weight loss is significantly higher in patients who underwent bypass surgery. Most comprehensive studies show that this difference in weight loss is preserved for at least 5 years. The data regarding measures other than weight loss are less robust, but the findings suggest that more patients would be cured of their diabetes, hypertension and other obesity-associated comorbidities if treated with bypass rather than banding. When asked, patients who underwent bypass generally appeared more satisfied than those who underwent banding. However, early complications (reflected in longer initial hospitalizations and greater early reoperation rates) were observed more commonly in the bypass groups; long-term complication rates were more common in bypass. It remains difficult to precisely assess the relative risks and benefits of the 2 procedures, and further studies are required for a firm judgment.
In conclusion, since obesity type 3 could seriously affect patients’ well-being, bariatric surgeries are usually suggested in this situation. The choice of the type of the surgery strongly depends on patients’ conditions. If a patient is strongly motivated to follow after-surgery instructions and control his/her food consumption and exercise, then banding surgery might be a good choice. Otherwise, bypass which offers quicker outcome, more persistent results, less failure rate and higher potential for resolution of comorbidities would be a better choice, although changes made in the organs is extremely difficult to reverse in this case.
References
[1] Tice, J.A., Karliner, L., Walsh, J., Petersen, A.J., Feldman, M.D., “Gastric banding or bypass? A systematic review comparing the two most popular bariatric procedures”, The American journal of medicine, vol. 121, no. 10, pp. 885-893, 2008.
[2] Romy, S., Donadini, A., Giusti, V., Suter, M., “Roux-en-Y gastric bypass vs gastric banding for morbid obesity: a case-matched study of 442 patients”, Archives of Surgery, 2011.
[3] http://www.nwwls.com/band-versus-bypass-weight-loss-surgeries
